24 results
The kynurenine pathway in schizophrenia, bipolar disorder, and major depressive disorder: a systematic review and meta-analysis of cerebrospinal fluid studies
- E. Salagre, B. S. Fernandes, M. E. Inam, I. Grande, E. Vieta, J. Quevedo, Z. Zhao
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S620
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The kynurenine pathway has been suggested to be involved in the pathophysiology of psychiatric disorders, including schizophrenia (SZ), bipolar disorder (BD), and major depressive disorder (MDD).
ObjectivesTo conduct a systematic review and meta-analysis of the kynurenine pathway metabolites from cerebrospinal fluid samples in SZ, BD, and MDD.
MethodsPubMed and Scopus databases were searched from inception to April 2022 to identify case-control studies assessing kynurenine metabolites [tryptophan (TRP), kynurenine (KYN), kynurenic acid (KA), quinolinic acid (QA), and 3-hydroxykynurenine (3-HK)] in SZ, BD, and MDD vs. healthy controls (HC). PRISMA guidelines were followed in the literature review. The random effects model parameter was selected when comparing the standardized mean differences (SMD) between groups.
ResultsA total of 23 articles met inclusion criteria (number of articles k=8, 8, 11 for SZ, BD, and MDD, respectively). For SZ, KA levels were increased in SZ compared to HC (SMD=2.64, CI=1.16-4.13, p=0.0005, I2=96%, k=6, n=384). KYN levels were not significantly different between SZ and HC (SMD=4.19, CI=-0.70 to 9.09, p=0.0933, I2=99%, k=4, n=188). For BD, TRP levels (k=7) did not differ significantly between BD and HC. There was a limited number of studies to conclude increased levels of KA in BD (k=2). For MDD, although some studies tended toward increased levels of KYN in those with remission vs. decreased levels in those with current depression, there were no significant differences in any of the kynurenine metabolite levels. There was a limited number of studies to conclude increased levels of QA in MDD (k=2).
ConclusionsKA, which has possibly neuroprotective effects, is increased in SZ. QA, which has neurotoxic effects, may be increased in MDD. There may be alterations in this pathway based on population characteristics and mood states.
Disclosure of InterestE. Salagre: None Declared, B. Fernandes: None Declared, M. Inam: None Declared, I. Grande Grant / Research support from: Spanish Ministry of Science and Innovation (MCIN) (PI19/00954) integrated into the Plan Nacional de I+D+I and cofinanced by the ISCIII-Subdireccion General de Evaluacion y el Fondos Europeos de la Unión Europea (FEDER, FSE, Next Generation EU/Plan de Recuperación Transformación y Resiliencia_PRTR); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); and the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), CERCA Programme / Generalitat de Catalunya as well as the Fundació Clínic per la Recerca Biomèdica (Pons Bartran 2022-FRCB_PB1_2022), Paid Instructor of: ADAMED, Angelini, Casen Recordati, Ferrer, Janssen Cilag, and Lundbeck, Lundbeck-Otsuka, Luye, SEI Healthcare , E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI15/00283, PI18/00805) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357, Paid Instructor of: AB-Biotics, AbbVie, Angelini, Biogen, Boehringer-Ingelheim, Celon Pharma, Dainippon Sumitomo Pharma, Ferrer, Gedeon Richter, GH Research, Glaxo-Smith Kline, Janssen, Lundbeck, Novartis, Orion Corporation, Organon, Otsuka, Sage, Sanofi-Aventis, Sunovion, and Takeda, J. Quevedo: None Declared, Z. Zhao: None Declared
Precision in bipolar disorders
- I. Grande
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S5
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Abstract
In many fields of heath, precision medicine has been integrated in clinical practise, for instance in oncology. In the case of psychiatry, and in particular bipolar disorder, we are in a prior step for the moment. Different proposal of stratification will be described during the talk for instance the classification of staging. Moreover some proposal of precision psychiatry in bipolar disorder will be put forward.
Disclosure of InterestNone Declared
Does bipolar disorder differ from other mental illnesses in terms of emotion dysregulation? A systematic review and meta-analysis
- M. De Prisco, V. Oliva, G. Fico, J. Radua, I. Grande, N. Roberto, G. Anmella, D. Hidalgo-Mazzei, M. Fornaro, A. de Bartolomeis, A. Serretti, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S571-S572
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Emotion regulation (ER) is the ability to assess, monitor, or modify emotional reactions to achieve a goal (Gross. Psychological inquiry 2015; 26 1-26). When ER strategies are rigidly or maladaptively applied, emotional dysregulation (ED) can occur (Thompson. Development and psychopathology 2019; 31 805-815). ED is common in people diagnosed with bipolar disorder (BD), but it can also be described in other clinical populations given its transdiagnostic nature. Numerous aspects of ED have been described in BD (De Prisco et al. Neuroscience & Biobehavioral Reviews 2022; 104914), but it is unclear whether these manifest similarly in other conditions such as major depressive disorder (MDD) or borderline personality disorder (BPD), or whether they are specific to BD.
ObjectivesThe objective of this systematic review and meta-analysis is to examine the literature comparing BD with other psychiatric disorders in terms of ED, focusing on those studies using validated clinical tools.
MethodsA systematic search from inception to April 28th, 2022, was conducted exploring the PubMed/MEDLINE,EMBASE, Scopus, and PsycINFO databases. Those studies providing quantitative data on ED in people diagnosed with BD and compared with clinical groups were eligible for inclusion. No restriction about age, sample size, or language were applied. Random effect meta-analyses were conducted, and effect sizes were calculated as standardized mean differences (SMD).
ResultsA total of 3,239 records was identified and, after duplicate removal and title/abstract evaluation, 112 were explored at the full text. Twenty-nine studies were finally included, and it was possible to perform a meta-analysis with twenty-two (145 comparisons) of them. Only studies comparing BD with MDD, and BPD provided sufficient data to perform a meta-analysis. People with BD did not differ from people with MDD in most of the comparisons considered. However, BD patients presented higher positive rumination (two comparisons: SMD=0.46; CI=0.27, 0.64; p=8.5e-07; I2=0%; and SMD=0.34; CI=0.15, 0.52; p=2.7e-04; I2=0%) and risk-taking behaviors (SMD=0.48; CI=0.27, 0.69; p=8.11e-06; I2=0%). In contrast, people with BPD displayed an overall higher degree of ED (SMD=-1.22; CI=-1.94, -0.5; p=9.1e-04; I2= 90.7) and used fewer adaptive ER strategies. Additionally, higher levels of self-blaming (SMD=-0.80; CI=-1.11, -0.50; p=2.68e-07; I2=0) and impulsive behavior (SMD=-0.76; CI=-0.89, -0.63; p=5.4e-29; I2=0) were observed.
Image:
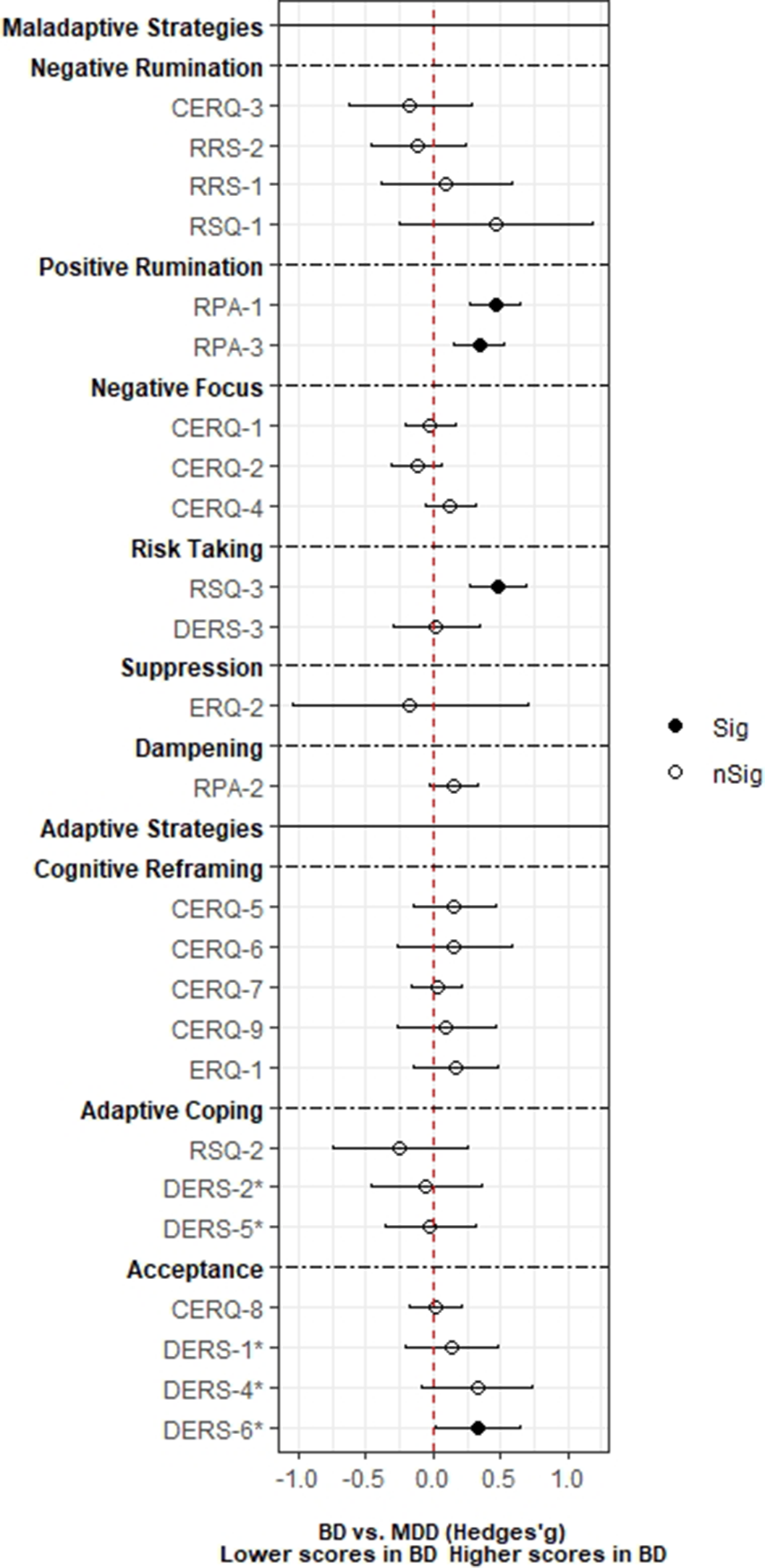
Image 2:
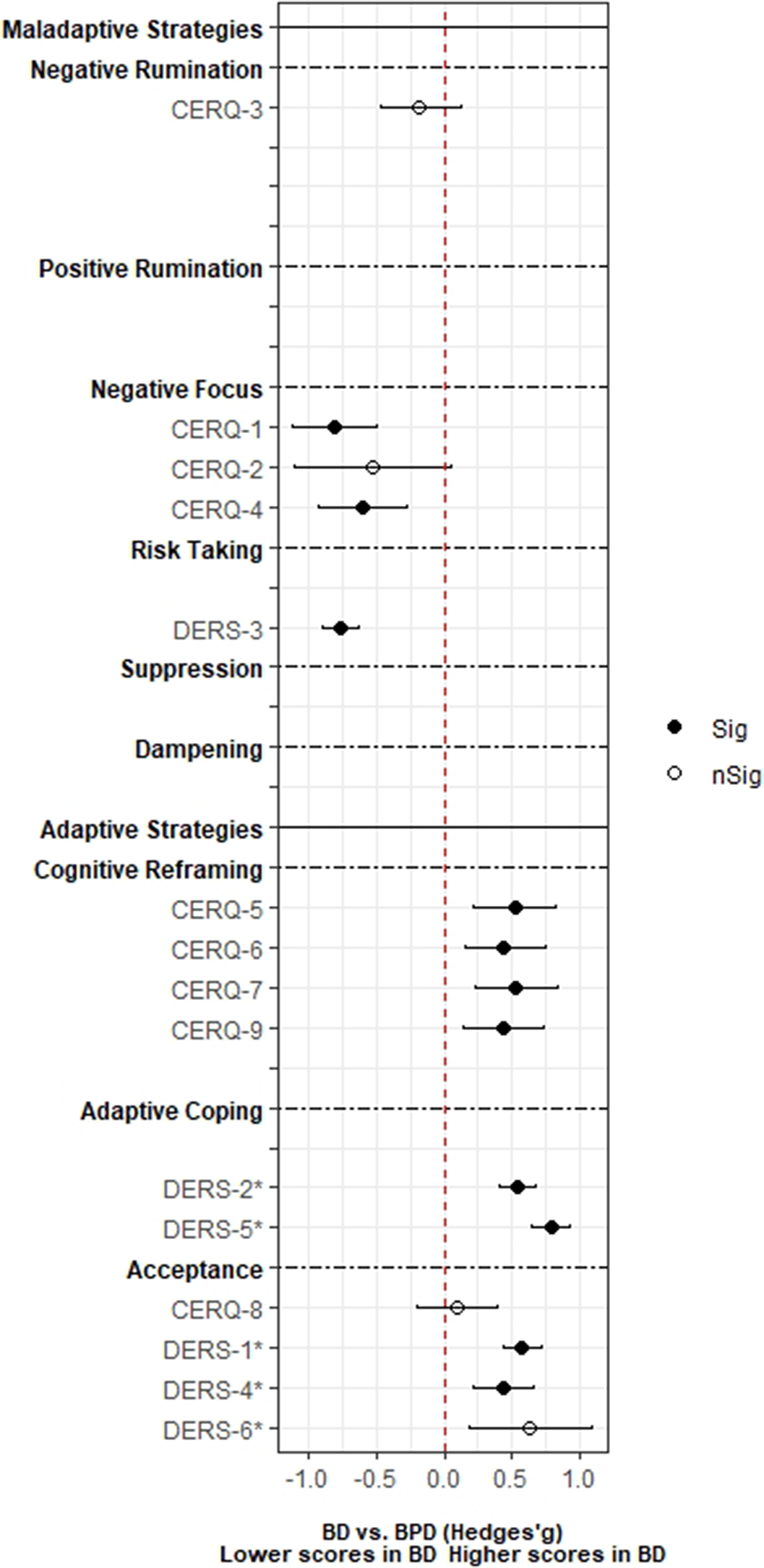 Conclusions
ConclusionsED is a trans-diagnostic construct that spans a continuum of different psychiatric disorders. Outlining the specific clinical features of one disorder versus another may help future research to increase our knowledge of these issues and develop new treatment strategies to reduce the clinical burden of these patients.
Disclosure of InterestM. De Prisco: None Declared, V. Oliva: None Declared, G. Fico Grant / Research support from: “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), Consultant of: Angelini, Janssen-Cilag and Lundbeck, J. Radua Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00394, CPII19/00009) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER) and the Instituto de Salud Carlos III, I. Grande Grant / Research support from: Spanish Ministry of Science and Innovation (MCIN) (PI19/00954) integrated into the Plan Nacional de I+D+I and cofinanced by the ISCIII-Subdirección General de Evaluación y el Fondos Europeos de la Unión Europea (FEDER, FSE, Next Generation EU/Plan de Recuperación Transformación y Resiliencia_PRTR ); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); and the the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), CERCA Programme / Generalitat de Catalunya as well as the Fundació Clínic per la Recerca Biomèdica (Pons Bartran 2022-FRCB_PB1_2022), Consultant of: ADAMED, Angelini, Casen Recordati, Ferrer, Janssen Cilag, and Lundbeck, Lundbeck-Otsuka, Luye, SEI Healthcare, N. Roberto: None Declared, G. Anmella Grant / Research support from: Rio Hortega 2021 grant (CM21/00017) from the Spanish Ministry of Health financed by the Instituto de Salud Carlos III (ISCIII) and co-financed by the Fondo Social Europeo Plus (FSE+), Consultant of: Janssen-Cilag, Lundbeck, Lundbeck/Otsuka, and Angelini, D. Hidalgo-Mazzei Grant / Research support from: Juan Rodés JR18/00021 granted by the Instituto de Salud Carlos III (ISCIII), M. Fornaro: None Declared, A. de Bartolomeis Consultant of: Janssen, Lundbeck, and Otsuka and lecture fees for educational meeting from Chiesi, Lundbeck, Roche, Sunovion, Vitria, Recordati, Angelini and Takeda; he has served on advisory boards for Eli Lilly, Jansen, Lundbeck, Otsuka, Roche, and Takeda, Chiesi, Recordati, Angelini, Vitria, A. Serretti Consultant of: Abbott, Abbvie, Angelini, AstraZeneca, Clinical Data, Boehringer, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Innovapharma, Italfarmaco, Janssen, Lundbeck, Naurex, Pfizer, Polifarma, Sanofi, Servier, and Taliaz, E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/00805, PI21/00787) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357. Thanks the support of the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151), Consultant of: AB-Biotics, AbbVie, Angelini, Biogen, Boehringer-Ingelheim, Celon Pharma, Dainippon Sumitomo Pharma, Ethypharm, Ferrer, Gedeon Richter, GH Research, Glaxo-Smith Kline, Janssen, Lundbeck, Medincell, Novartis, Orion Corporation, Organon, Otsuka, Rovi, Sage, Sanofi-Aventis, Sunovion, Takeda, and Viatris, A. Murru Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00672) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), Consultant of: Angelini, Idorsia, Lundbeck, Pfizer, Takeda
Vickybot, a chatbot for anxiety-depressive symptoms and work-related burnout
- G. Anmella, M. Sanabra, M. Primé-tous, X. Segú, M. Cavero, R. Navinés, A. Mas, V. Olivé, L. Pujol, S. Quesada, C. Pio, M. Villegas, I. Grande, I. Morilla, A. Martínez-Aran, V. Ruiz, E. Vieta, D. Hidalgo-Mazzei
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S109-S110
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A significant proportion of people attending Primary Care (PC) have anxiety-depressive symptoms and work-related burnout and there is a lack of resources to attend them. The COVID-19 pandemic has worsened this problem, particularly affecting healthcare workers, and digital tools have been proposed as a workaround.
ObjectivesWe present the development, feasibility and effectiveness studies of chatbot (Vickybot) aimed at screening, monitoring, and reducing anxiety-depressive symptoms and work-related burnout in PC patients and healthcare workers.
MethodsUser-centered development strategies were adopted. Main functions included self-assessments, psychological modules, and emergency alerts. (1) Simulation: HCs used Vickybot for 2 weeks to simulate different possible clinical situations and evaluated their experience. (3) Feasibility and effectiveness study: People consulting PC or healthcare workers with mental health problems were offered to use Vickybot for one month. Self-assessments for anxiety (GAD-7) and depression (PHQ-9) symptoms, and work-related burnout (based on the Maslach Burnout Inventory) were administered at baseline and every two weeks. Feasibility was determined based on the combination of both subjective and objective user-engagement Indicators (UEIs). Effectiveness was measured using paired t-tests as the change in self-assessment scores.
Results(1) Simulation: 17 HCs (73% female; mean age=36.5±9.7) simulated different clinical situations. 98.8% of the expected modules were recommended according to each simulation. Suicidal alerts were correctly activated and received by the research team. (2) Feasibility and effectiveness study: 34 patients (15 from PC and 19 healthcare workers; 77% female; mean age=35.3±10.1) completed the first self-assessments, with 34 (100%) presenting anxiety symptoms, 32 (94%) depressive symptoms, and 22 (64.7%) work-related burnout. Nine (26.5%) patients completed the second self-assessments after 2-weeks of use. No significant differences were found for anxiety [t(8) = 1.000, p = 0.347] or depressive [t(8) = 0.400, p = 0.700] symptoms, but work-related burnout was significantly reduced [t(8) = 2.874, p = 0.021] between the means of the first and second self-assessments. Vickybot showed high subjective-UEIs, but low objective-UEIs (completion, adherence, compliance, and engagement).
ConclusionsThe chatbot proved to be useful in screening the presence and severity of anxiety and depressive symptoms, in reducing work-related burnout, and in detecting suicidal risk. Subjective perceptions of use contrasted with low objective-use metrics. Our results are promising, but suggest the need to adapt and enhance the smartphone-based solution in order to improve engagement. Consensus on how to report UEIs and validate digital solutions, especially for chatbots, are required.
Disclosure of InterestNone Declared
Psychiatric comorbidity profiles among suicidal attempters: A cohort study
- Y. Sanchez-Carro, M. Diaz-Marsa, V. Fernandez-Rodrigues, W. Ayad-Ahmed, A. Pemau, I. Perez-Diaz, A. Galvez-Merlin, P. de la Higuera-Gonzalez, V. Perez-Sola, P. Saiz, I. Grande, A. Cebria, J. Andreo-Jover, P. Lopez-Peña, M. Ruiz-Veguilla, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S318-S319
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
More than 700,000 people die by suicide in 2019 globally (World Health Organitation 2021). Mental health problems constitute a risk factor for suicidal behavior and death by suicide (Hoertel et al. Mol Psychiatry 2015; 20 718–726). Different mental disorders have been related to different forms of suicidal ideation and behavior (Conejero et al. Curr Psychiatry Rep 2018; 20, 33) (Quevedo et al. Compr Psychiatry 2020; 102 152194). However, little is known on comorbidity profiles among suicide attempters.
ObjectivesThe aim of our work was to identify the psychiatric comorbidity profiles of individuals who were admitted a hospital emergency department due to a suicide attempt. Moreover, it intended to know their clinical characteristics according to comorbidity profile.
MethodsA sample of 683 attempters (71.30% female; M age= 40.85, SD= 15.48) from the SURVIVE study was used. Patients were assessed within the 15 days after emergency department admission. Sociodemographic (i.e., sex, age, marital status and employment status) and clinical data were collected. The International Neuropsychiatric Interview (MINI) was used to assess DSM-V Axis 1 mental health diagnoses and the Columbia Suicide Rating Scale (C-SSRS) to assess suicidal ideation and behavior. The Acquired Capacity for Suicide-Fear of Death Scale (ACSS-FAD), the Patient Health Questionnaire (PHQ-9) to assess the frequency of depressive symptoms during the past 2 weeks, and the General Anxiety Disorder-7 (GAD-7) scale to assess symptoms of worry and anxiety were also conducted. For the identification of comorbidity profiles, latent class analysis framework was followed considering diagnosis to each individual disorder as clustering variables. On the other hand, binary logistic regression was used to study the relationship between comorbidity profile membership and clinical factors.
ResultsTwo classes were found (Class I= mild symptomatology class, mainly featured by emotional disorder endorsement; and Class II= high comorbidity class, featured by a wide amount of endorsed diagnoses) (see figure 1). Individuals from the High comorbidity class were more likely to be female (OR= 0.98, p<.05), younger in age (OR= 0.52, p< .01), with more depressive symptoms (OR=1.09, p<.001) and have greater impulsivity (OR= 1.01, p<.05).
Image:
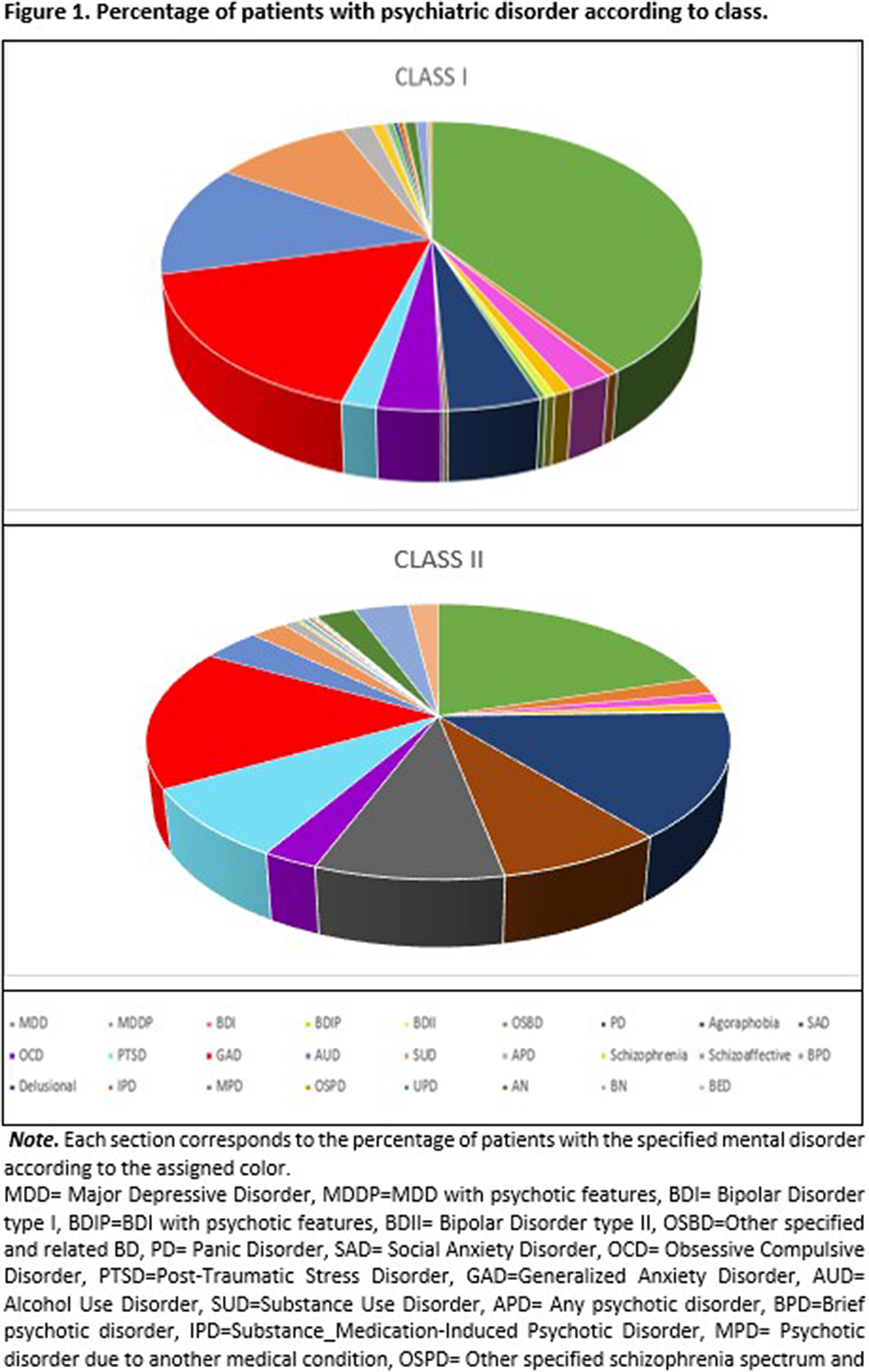 Conclusions
ConclusionsWe found two profiles of people with suicidal behavior based on the presence of mental disorders. Each of the suicidal subtypes had different associated risk factors. They also had a different profile of suicidal behavior.
Disclosure of InterestNone Declared
Parkinson’s Disease and Bipolar Disorder: a case report and narrative review
- H. Andreu Gracia, L. Ilzarbe, O. Marco Estrada, L. Bueno Sanya, O. De Juan Viladegut, L. Olivier Mayorga, L. Pintor, F. Valldeoriola, I. Grande
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S480
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar disorder (BD) is considered a risk factor for developing Parkinson’s Disease (PD) because of an altered dopamine activity in both entities. Comorbidity may delay diagnosis and difficult therapeutic management.
ObjectivesTo describe the case of a patient with both BD and PD and to determine the appropriate diagnostic and therapeutic approach for patients presenting both entities.
MethodsWe present the case of a 58-year-old woman attended in our neurology unit due to the initial presence of visual hallucinations as a core symptom.
ResultsPsychotic symptoms as hallucinations and off-times, frequently observed in PD, may be misdiagnosed with a worsening of depressive polarity of BD. Thus, overlap between symptoms may lead to a challenging differential diagnosis. Moreover, there is no consensus about the therapeutic management of the comorbidity, due to the bidirectional worsening of symptoms when treatment is adjusted. In our case, a diagnosis of dopaminergic psychosis was made so antipsychotic treatment with quetiapine 50 mg/d was initiated. A worsening of symptoms was observed, presenting the patient a stuporous status, mutism and generalized rigidity. Neuroimaging and lumbar puncture were performed showing no alterations; electroencephalogram showed diffuse slowing. Final diagnosis was an off-episode of PD and a multifactorial encephalopathy resulting in visual hallucinations.
ConclusionsCoexistence of PD and BD may lead to a diagnostic and therapeutic delay and therefore a worse prognosis. Although these diseases are well-known, it is still challenging to manage patients presenting both entities. Further research is needed to clarify the proper diagnostic and therapeutic approach for these patients.
DisclosureNo significant relationships.
P03-321 Antipsychotic Polipharmacy in Schizophrenic Inpatients
- A. Batalla, J. Undurraga, I. Grande, A. Pons
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E927
-
- Article
-
- You have access Access
- Export citation
-
Objectives
Concomitant antipsychotic prescription is common in clinical psychiatry, although it is not an evidence-based practice. The aim of the study was to describe the prescription of antipsychotics in inpatients with schizophrenia and identify which are the factors associated with this tendency.
MethodsWe reviewed retrospectively the psychotropic drugs prescribed at the time of discharge of 177 inpatients who met criteria for schizophrenia [DSM-IV-TR] on an acute psychiatry unit from 2007 to 2008.
ResultsOne hundred and two patients (57.6%) were male. Mean age (SD) was 38.1 (14.6) years. The percentage of patients discharged on treatment with two or more antipsychotics was 43.5%. Although in the strict sense we should not consider it as polipharmacy, the most frequent combination was long acting injectable risperidone with oral risperidone (21.5%), followed by long acting injectable typical antipsychotic with oral risperidone (3.4%). There was a significant association between the number of prescribed antipsychotics and the total number of previous hospitalizations and the number of hospitalizations during the previous year (ANOVA p=0.001 and p< 0.001 respectively). No correlation was found between polypharmacy and age. There was a significant association between the number of antipsychotics prescribed and the use of anticholinergic treatment (t-test p=0.005).
ConclusionsOur polypharmacy rates are comparable with prior European data (30-76%). Despite of the clinical guidelines, antipsychotic polipharmacy is an extended therapeutic strategy not necessarily related with resistant schizophrenia. Most of the antipsychotic associations identified are not evidenced-based practice. More clinical trials are needed to determine the efficacy of different combinations.
P03-333 - Electrocardiographic Alterations in Patients in Treatment with Clozapine
- I. Grande, A. Pons, Á. Torras, I. Baeza, M. Bernardo
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E939
-
- Article
-
- You have access Access
- Export citation
-
Objectives
Cardiovascular side effects of antipsychotics are been studied both in typical and atypical antipsychotics but, in particular, with clozapine few systematic studies of these effects have been performed. In this study, we reviewed electrocardiographic (ECG) data from patients treated with clozapine.
MethodsObservational, retrospective study in our Clozapine Day Clinic from 2000 to 2008. We recluted 197 patients (70% men) with mean age 31,75 ± 9,0 years who began treatment with clozapine. All of them had an electrocardiogram taken before starting treatment and after 18 weeks of follow-up. None suffered from heart diseases. QTc was evaluated by Bazett formula (QT/ (R-R’)1/2). Treatment prescribed was taken down and drug serum levels were detected. Statistical analysis was executed by SPSS 17.0.
ResultsThere was significant correlation between doses prescribed and levels of clozapine and norclozapine (r=.304, p=.023; r=.354 p=.007), between levels of clozapine, norclozapine and QTc enlargement (r=.348, p=.008; r=.268 p=.046) and between levels of clozapine, norclozapine and heart rate (r=.390, p=.003; r=.326 p=.014). There were no differences between QTc and treatment with clozapine or other antipsychotic (p=0.902), between sex or if polypharmacy existed. ECG alterations were a case of supraventricular extrasystoles, another of Wolf-Parkinson -White Syndrome and other inespecific alterations like repolarizations or left hypertrophy.
ConclusionWe did not find either major incidence on cardiological effects or significative QTc enlargement during treatment with clozapine in contrast to other antipsychotic previously prescribed. Therefore clozapine may be in the same cardiologic safety rank than other antipsychotics.
The burden of mental disorders in primary care
- G. Grandes, I. Montoya, M.S. Arietaleanizbeaskoa, V. Arce, A. Sanchez, on behalf of the MAS group
-
- Journal:
- European Psychiatry / Volume 26 / Issue 7 / October 2011
- Published online by Cambridge University Press:
- 16 April 2020, pp. 428-435
-
- Article
- Export citation
-
Objectives
To describe and compare the prevalence of mental disorders across primary care populations, and estimate their impact on quality of life.
MethodsCross-sectional multilevel analysis of a systematic sample of 2539 attendees to eight primary care centres in different regions of Spain, assessed with the WHO Composite International Diagnostic Interview (CIDI 1.1), the Short Form Health Survey (SF-36) quality of life questionnaire and the SF-6D utility index.
ResultsThe 12-month prevalence of any mental disorder was 23% (95% confidence interval: 21–24%), 10% had mood, 9% anxiety, 5% organic, 4% somatoform, and 1% alcohol use disorders, with a significant between-centre variability (P < 0.001). People with mental disorders had one standard deviation lower mental quality of life than the general population. We estimated that 1831 quality-adjusted life-years (QALYs) are lost annually per 100,000 patients due to mental disorders, without considering mortality. Mood disorders have the worst impact with an annual loss of 1124 QALYs per 100,000 patients, excluding mortality (95% confidence interval: 912–1351).
ConclusionsPrevalence rates were similar to those obtained in international studies using the same diagnostic instrument and, given the significant between-centre variability found, it is recommended that mental health statistics be considered at small area level. Mental disorders, and especially mood disorders, are associated with very poor quality of life and higher scores on disability indexes than other common chronic conditions.
Remission and functioning after two years undergoing Long-Acting Injectable Risperidone (LAIR) in recent-onset schizophrenia
- A. Batalla, A. Pons, A. Ortiz, I. Grande, J. Undurraga, E. Parellada
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 1344
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Improving adherence in the early stages of illness by means of long-acting antipsychotics can lead to reduced number of readmissions and enhanced remission rates, which could lead to improved performance in the medium-long term.
ObjectivesAssessing clinical remission, number of admissions and personal and social performance in recent-onset schizophrenic patients undergoing LAIR.
MethodsLongitudinal retrospective study of a cohort of thirty-one recent-onset schizophrenic patients ( ≤ 2 years) who started LAIR treatment between 2004–2008. Twenty-six (83.9%) were treated for two years. PANSS scale was assessed at baseline; PANSS, Personal and Social Performance scale (PSP) and remission criteria after two years.
ResultsTwenty-six patients (83.9%), 61.5% male aged between 16–44 years old, completed two years of treatment. All patients met criteria for schizophrenia (DSM-IV) with an average duration of 0.8 year since diagnosis. The main reason to using LAIR was poor adherence (76.9%). The PANSS total and all its subscale scores improved significantly (p < 0.005) with 80.8% of patients showing a ≥ 50% improvement on the PANSS total. Seventeen patients (65.4%) achieved remission criteria. Five patients (19.2%) were admitted during the follow-up. The average on global functioning (PSP) was 72.4 (IC 95%, 66.4-78.4). LAIR doses at baseline were 25 mg (46.2%), 37.5 mg (30.8%) or 50 mg (23.1%); after two years, 25 mg (34.6%), 37.5 mg (34.6%), 50 mg (23.1%) or 75 mg (7.7%).
ConclusionsDespite the limitation of retrospective observational studies, our data, including the good adherence rate (83.9%), suggest that LAIR could be effective in the treatment of recent-onset schizophrenia.
is the Brief Psychotic Disorder a Distinct Nosologic Entity?: A Longitudinal Study of 80 Patients
- L. Rodriguez Incio, I. Grande Fullana, V. Sánchez Gistau, M. Bernardo Arroyo, E. Parellada Rodón
-
- Journal:
- European Psychiatry / Volume 24 / Issue S1 / January 2009
- Published online by Cambridge University Press:
- 16 April 2020, 24-E1188
-
- Article
-
- You have access Access
- Export citation
-
Introduction:
The DSM-IV-TR category “brief psychotic disorder” includes different concepts that have been defined before like bouffée délirante, cycloid psychosis and “acute and transient psychosis” in the last ICD-10. Limited prospective studies have been done, and they all show a marked diagnostic instability during follow-up. According to that, its independent nosologic entity is still uncertain.
Aims:To determine the diagnostic stability of the brief psychotic disorders as well as their distinct clinical features.
Method:Observational, retrospective, longitudinal study of 80 consecutive patients admitted at the acute psychiatric inpatient service of a general hospital between 2000 and 2006. at discharge, all of them fulfilled diagnostic criteria for “brief psychotic disorder” according to DSM-IV. Demographic and psychopathological data were analysed.
Results:Mean age (SD) was 31.3 (9.5), most of them women (63%). the most frequent previous stressor was related to labour, while up to 45% didn't report any. 51% had no psychiatric family history. 15 (19%) patients previously had a brief psychotic episode. Psychopathological disturbances identified were: thought disorder 69%, anxiety 66.6%, insomnia 57.7%, suspiciousness 53.5%, rapidly changing delusions 53.3% (paranoid contents 75.3%), perplexity 46.5%, auditory hallucinations 45.1%, mood lability 36.6%, elation 23.9%, depressed mood 22.5% and irritability 12.7%. in the 24 month follow-up, 32.5% changed diagnosis to schizophrenia, 3"9% to schizoaffective, 10% to bipolar disorder and 16.9% achieved clinical remission. 28.5% were lost to follow-up.
Conclusion:“Brief psychotic disorder” category is still uncertain and more data may be necessary to clarify if it should remain as a distinct nosologic entity.
The Real World Costs of Asenapine in Manic Episodes in the Manacor Study
- I. Forcada, I. Grande, D. Hidalgo-Mazzei, E. Nieto, C. Saez, M. Mur, E. Vieta
-
- Journal:
- European Psychiatry / Volume 30 / Issue S1 / March 2015
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Background
Asenapine is the most recent compound that hasbeen FDA- and EMA-approved for treatment of mania. Its efficacy and safety havebeen assessed in placebo-controlled trials, but little is known about itsperformance in routine clinical conditions. The MANACOR study assessed costsassociated with treatment of mania in several hospital settings acrossCatalonia, Spain. As part of the protocol, we compared cost-effectiveness ofasenapine versus other treatment options.
MethodsA combined prospective and retrospective datacollection and analysis was conducted from January 2011 to December 2013following a clinical interview and assessment of manic and depressive symptoms(YMRS, HDRS-17), clinical state (CGI-BP-M), psychosocial functioning (FAST),sexual dysfunction (PRSexDQ) and health resource costs associated withtreatment with asenapine versus other antipsychotics.
Results152 patients from different university hospitalswere included. 53 patients received asenapine and 99 received otherantipsychotics. Considering inpatients (N=117), those treated with asenapinepresented a significantly less severe manic episode (p=0.001), less psychoticsymptoms (p=0.030) and, more comorbid personality disorder (p=0.002). Regardingoutpatients, those treated with asenapine showed significantly less severemanic episode (p=0.046), more previous mixed episodes (p= 0.013) and, moresexual dysfunction at baseline (p=0.036). No significant differences were foundin mean total costs per day.
LimitationsNon-randomized study design.
ConclusionClinicians tended to use asenapine in patientswith less severe manic symptoms but more complex clinical profile, includingmore mixed episodes in the past, concomitant personality disorder, and sexualproblems. Treatment with asenapine was not associated with higher costs when comparedto other options.
Asenapine prescribing patterns in the treatment of manic in- and outpatients: Results from the MANACOR study
- I. Grande, D. Hidalgo-Mazzei, E. Nieto, M. Mur, C. Sàez, I. Forcada, E. Vieta
-
- Journal:
- European Psychiatry / Volume 30 / Issue 4 / June 2015
- Published online by Cambridge University Press:
- 15 April 2020, pp. 528-534
-
- Article
- Export citation
-
Background:
Asenapine is the most recent compound that has been FDA- and EMA-approved for treatment of mania. Its efficacy and safety have been assessed in placebo-controlled trials, but little is known about its performance in routine clinical conditions. In this study, we compared features of patients treated with adjunctive asenapine or other adjunctive antipsychotics and the costs of the treatment.
Methods:A combined prospective and retrospective data collection and analysis was conducted from January 2011 to December 2013 following a clinical interview and assessment of manic and depressive symptoms (YMRS, HDRS-17), clinical state (CGI-BP-M), psychosocial functioning (FAST), sexual dysfunction (PRSexDQ) and health resource costs associated with treatment with adjunctive asenapine versus other adjunctive antipsychotics.
Results:Hundred and fifty-two patients from different university hospitals were included. Fifty-three patients received adjunctive asenapine and 99 received other adjunctive antipsychotics concomitantly to mood stabilizers. Considering inpatients, those treated with adjunctive asenapine presented a significantly less severe manic episode (P = 0.001), less psychotic symptoms (P = 0.030) and more comorbid personality disorder (P = 0.002). Regarding outpatients, those treated with adjunctive asenapine showed significantly less severe manic episode (P = 0.046), more previous mixed episodes (P = 0.013) and more sexual dysfunction at baseline (P = 0.036). No significant differences were found in mean total costs per day.
Conclusion:Clinicians tended to use adjunctive asenapine in patients with less severe manic symptoms but more complex clinical profile, including more mixed episodes in the past, concomitant personality disorder, and sexual problems. Treatment with adjunctive asenapine was not associated with higher costs when compared to other options.
P-179 - Brain-derived Neurotrophic Factor as a Biomarker of Clinical Response in Bipolar Disorder: 16 Week Follow-up Study
- I. Grande, I. Chendo, B.N. Frey, K.M. Cereser, L. Stertz, G. Colpo, G.R. Fries, A.B. da Cunha, E. Vieta, F. Kapczinski
-
- Journal:
- European Psychiatry / Volume 27 / Issue S1 / 2012
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Despite therapeutic advances, we still have difficulties in predicting response to treatment in bipolar disorder (BD). Brain-Derived Neurotrophic Factor (BDNF) has been put forward as a potential peripheral marker of treatment response.
ObjectiveTo prospectively study the relation between clinical response to treatment and serum BDNF levels.
AimsTo investigate a) a possible association between serum BDNF levels and clinical response along 16 week follow-up and b) the role of val66met polymorphism in clinical response in a sample of drug-free patients with BD going through a mood episode.
MethodsThis is a naturalistic, open-label prospective nested case control study matched for age, gender and ethnicity. Patients were 18 years or older, required BD diagnosis, undergoing a current manic, mixed or depressive episode and be off-medication for at least 2 weeks. Clinical assessment and blood withdrawn were conducted along follow-up. At the end of the study, patients were classified according to clinical response.
Results25 of 36 (69.4%) of the patients were female and the mean age was 37.8 (SD 11.8) years old. Baseline serum BDNF levels did not show any difference between patients and controls (p = 0.075).There was a significant negative correlation between differences in serum BDNF levels and in CGI score along follow-up (r = −.372, p = 0.028). Serum BDNF levels were significant higher in responders compared to non-responders at week 4, 8 and 16 (p = 0.026, p = 0.009, p = 0.001 respectively). Val66met polymorphism did not seem to interfere in clinical response.
ConclusionsChanges in serum BDNF levels may help in monitoring treatment response.
1588 – Interleukin-6 As a Biomarker Of The Model Of Staging In Bipolar Disorder
- I. Grande, P.V. Magalhaes, I. Chendo, L. Stertz, C.S. Gama, E. Vieta, F. Kapczinski
-
- Journal:
- European Psychiatry / Volume 28 / Issue S1 / 2013
- Published online by Cambridge University Press:
- 15 April 2020, 28-E874
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Different proposals of the staging model in bipolar disorder (BD) have been launched suggesting a progression from prodromal to more severe and refractory presentations. Biochemical variations in BD are receiving attention as they may help to understand the neurobiological correlates of the disorder and its neuroprogression.
ObjectivesStudy pro-inflammatory factors, such as interleukins along the progression of the disorder.
AimsTo investigate a) the role of interleukin-6 (IL-6) in the model of staging and b) to detect clinical predictors of variations in IL-6 levels.
MethodsThis is a case-control study matched for age and gender. Patients required the diagnosis confirmation by SCID, being in euthymia (HDRS, YMRS scores ≤ 7 in last month), and were classified in Kapczinski et al. clinical stages. At the end, 109 patients and 25 controls were eligible for the study. Serum IL-6 levels were determined by ELISA.
ResultsSeventy-six (69.7%) patients were female and the mean age was 44.2 (SD= 12.9) years. A significant increase in IL- 6 was found in patients compared to controls (t=2.33, p=0.02) and among the four groups of patients (F=2.85, p=0.04). Results from linear regression analysis revealed that number of episodes per year, age at first episode, and age were significantly associated with IL-6 (β=0.025, CI: 0.005-0.044, p=0.012; β=-0.016, CI:(-0.031)-(-0.001),p=0.033; β=0.042, CI:0.027-0.058, p=0.0001, respectively).
ConclusionsInterleukin-6 may be a useful biomarker in the model of staging in bipolar disorder and could be related to the number of episode per year and early onset of the disorder.
High Cognitive Reserve in Bipolar Disorders as a Moderator of Neurocognitive Impairment
- I. Grande, J. Sanchez-Moreno, B. Solé, E. Jimenez, C. Torrent, C.D.M. Bonnin, C. Varo, R. Tabarés-Seisdedos, V. Balanza-Martínez, E. Valls, I. Morilla, A.F. Carvalho, J.L. Ayuso-Mateos, E. Vieta, A. Martinez-Aran
-
- Journal:
- European Psychiatry / Volume 41 / Issue S1 / April 2017
- Published online by Cambridge University Press:
- 23 March 2020, p. S116
-
- Article
-
- You have access Access
- Export citation
-
Background
Cognitive reserve (CR) reflects the capacity of the brain to endure neuropathology, minimize clinical manifestations and successfully complete cognitive tasks. The present study aims to determine whether high CR may constitute a moderator of cognitive functioning in bipolar disorder (BD).
MethodsOne hundred and two patients with BD and 32 healthy controls were enrolled. All patients met DSM-IV criteria for I or II BD and were euthymic (YMRS ≤ 6 and HDRS ≤ 8) during a 6-month period. All participants were tested with a comprehensive neuropsychological battery, and a Cerebral Reserve Score (CRS) was estimated. Subjects with a CRS below the group median were classified as having low CR, whereas participants with a CRS above the median value were considered to have high CR.
ResultsParticipants with BD with high CR displayed a better performance in measures of attention (digits forward: F = 4.554, P = 0.039); phonemic and semantic verbal fluency (FAS: F = 9.328, P = 0.004; and Animal Naming: F = 8.532, P = 0.006); and verbal memory (short cued recall of California Verbal Learning Test: F = 4.236, P = 0.046), after multivariable adjustment for potential confounders, including number of admissions and prior psychotic symptoms.
ConclusionsHigh cognitive reserve may therefore be a valuable construct to explore for predicting neurocognitive performance in patients with BD regarding premorbid status.
Disclosure of interestDr. I. Grande has received a Juan Rodés Contract (JR15/00012), Instituto de Salud Carlos III, Spanish Ministry of Economy and Competiveness, Barcelona, Spain and has served as a consultant for Ferrer and as a speaker for AstraZeneca, Ferrer and Janssen-Cilag.
Disclosure of interestDr. I. Grande has received a Juan Rodés Contract (JR15/00012), Instituto de Salud Carlos III, Spanish Ministry of Economy and Competiveness, Barcelona, Spain and has served as a consultant for Ferrer and as a speaker for AstraZeneca, Ferrer and Janssen-Cilag.
Staging in Bipolar Disorder: Clinical, Biochemical, and Functional Correlates
- I. Grande
-
- Journal:
- European Psychiatry / Volume 41 / Issue S1 / April 2017
- Published online by Cambridge University Press:
- 23 March 2020, p. S34
-
- Article
-
- You have access Access
- Export citation
-
In the field of bipolar disorder, some proposals of a staging model have been suggested considering the progressive features of the disorder. The staging model regards special features of the patients and further draws a route to define the prognosis and treatment as well as the neurobiological background of the disorder. The aim of this model is to identify rational therapeutic targets and provide the most effective and less toxic intervention in a time-sensitive manner. Advocating for a model of staging in bipolar disorder that can group the patients according to quantitative cut-offs of common practice clinical variables as well as defining a biochemical correlation seems to be a further step towards an operative and valid model of staging in bipolar disorder.
Disclosure of interestDr. I. Grande has received a Juan Rodés Contract (JR15/00012), Instituto de Salud Carlos III, Spanish Ministry of Economy and Competiveness, Barcelona, Spain and has served as a consultant for Ferrer and as a speaker for AstraZeneca, Ferrer and Janssen-Cilag.
Use of benzodiazepines and cognitive performance in primary care patients with first cognitive complaints
- G. Grande, I. Tramacere, D. L. Vetrano, S. Pomati, C. Mariani, G. Filippini
-
- Journal:
- International Psychogeriatrics / Volume 30 / Issue 4 / April 2018
- Published online by Cambridge University Press:
- 10 November 2017, pp. 597-601
-
- Article
- Export citation
-
The aim of the present study is to investigate the impact of benzodiazepine use on cognitive performance in primary care patients with first cognitive complaints. The association between the exposition to benzodiazepines (short and long half-life) and cognitive performance, evaluated through the Mini Mental State Examination (MMSE), was tested through analysis of the covariance and logistic regression models. Within the 4,249 participants (mean age 77.0 ± 8.2, 66.4% women), 732 (17%) were on benzodiazepines. When compared with non-users, short- and long-acting benzodiazepine users presented overlapping adjusted MMSE mean scores (respectively, mean MMSE score: 25.3, 95%CI 25.2–25.5; 25.4, 95%CI 25.1–25.7, and 25.9, 95%CI 25.3–26.4; p = 0.156). When tested according to the logistical regression model, after adjusting for potential confounders, no association was found between short and long acting benzodiazepine use and a MMSE < 24 (respectively, OR 0.9, 95%CI 0.7–1.2; OR 0.8, 95%CI 0.7–1.3) as compared with non-users. In conclusion, according to the results of our study, benzodiazepine use seems not to impact on cognitive performance- as assessed with the MMSE- of primary care patients referring to GPs for first cognitive complaints.
The Clinical Implications Of Cognitive Impairment and Allostatic Load in Bipolar Disorder
- E. Vieta, D. Popovic, A.R. Rosa, B. Solé, I. Grande, B.N. Frey, A. Martinez-Aran, J. Sanchez-Moreno, V. Balanzá-Martínez, R. Tabarés-Seisdedos, F. Kapczinski
-
- Journal:
- European Psychiatry / Volume 28 / Issue 1 / January 2013
- Published online by Cambridge University Press:
- 24 April 2012, pp. 21-29
-
- Article
- Export citation
-
Background
Allostatic load (AL) relates to the neural and bodily “wear and tear” that emerge in the context of chronic stress. This paper aims to provide clinicians with a comprehensive overview of the role of AL in patophysiology of bipolar disorder (BD) and its practical implications.
MethodsPubMed searches were conducted on English-language articles published from 1970 to June 2011 using the search terms allostatic load, oxidative stress, staging, and bipolar disorder cross-referenced with cognitive impairment, comorbidity, mediators, prevention.
ResultsProgressive neural and physical dysfunction consequent to mood episodes in BD can be construed as a cumulative state of AL. The concept of AL can help to reconcile cognitive impairment and increased rates of clinical comorbidities that occur over the course of cumulative BD episodes.
ConclusionsData on transduction of psychosocial stress into the neurobiology of mood episodes converges to the concept of AL. Mood episodes prevention would not only alleviate emotional suffering, but also arrest the cycle of AL, cognitive decline, physical morbidities and, eventually, related mortality. These objectives can be achieved by focusing on effective prophylaxis from the first stages of the disorder, providing mood-stabilizing agents and standardized psychoeducation and, potentially, addressing cognitive deficits by the means of specific medication and neuropsychological interventions.
High power laser development and experimental applications to X-ray lasers, and short pulse energy transport
- M. H. Key, H. Baldis, D. Brown, M. Grande, C. Hooker, Y. Kato, C. Lewis, P. Norreys, D. O'Neill, G. Pert, S. Ramsden, C. Regan, S. Rose, I. Ross, M. Shaw, G. Tallents, E. Wooding
-
- Journal:
- Laser and Particle Beams / Volume 8 / Issue 1-2 / January 1990
- Published online by Cambridge University Press:
- 09 March 2009, pp. 19-25
-
- Article
- Export citation
-
University research in the UK with high power lasers is carried out at the SERC's Central Laser Facility with a multi-terawatt neodymium glass laser, VULCAN, and a developmental KrF laser, SPRITE. These systems are briefly described together with the design of a new KrF laser to supersede VULCAN. The new laser design, SUPERSPRITE, is based on optical and Raman multiplexing which is being developed with the present SPRITE system. The specification of SUPERSPRITE is for 3.5 kJ in 1 ns and a peak power of 300 TW in short pulses. The new technology is seen as highly cost effective in relation to neodymium glass lasers. A resume of the development of XUV lasers in the UK in collaboration with laboratories overseas is given. The work is based on laser action through recombination in highly ionized ions and recent progress includes collaborative experiments on the GEKKO XII facility in Japan which have demonstrated laser action at the shortest wavelength to date at 45 A in Mg XII. The physics of energy transport in short pulses is fundamental to the extrapolation of recombination lasers to shorter wavelengths and is being studied from a more basic standpoint using both the VULCAN and SPRITE facilities. Some details of this work are given.






